If you’ve ever felt your stomach drop before a big meeting, or noticed your anxiety get worse after a weekend of bad food, you’ve already felt the gut-brain axis. You just didn’t have a name for it.
Most people try to fix anxiety by working on their mind. Therapy. Breathing. Meditation. Those things help. But almost nobody tells you that the bacteria living in your gut may be making your anxiety worse every single day.
Here’s what you’ll learn in this guide. What the gut-brain axis is, in plain English. Why 95% of your body’s serotonin is made in your gut, not your brain. What foods and daily habits can calm this system down. And a simple 4-week plan you can start this week.
This is not theory. The research is real. The steps are simple. Let’s get into it.
What Is the Gut-Brain Axis? (The Part Most Doctors Skip)
Your gut and brain are talking to each other right now. Not in a vague, feel-good way. Through real biological pathways — nerves, hormones, immune signals, and chemical messengers.
This communication system is called the gut-brain axis. It links your digestive tract directly to your central nervous system.
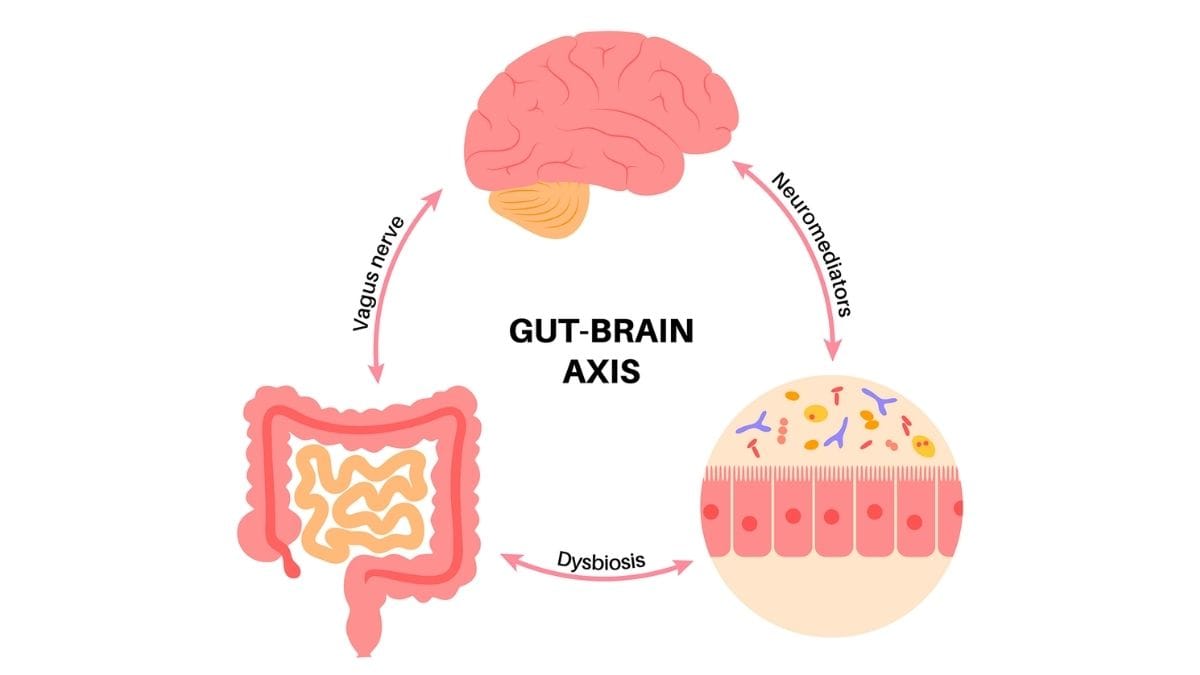
Inside your gut, there are over 100 million nerve cells. Scientists call this the enteric nervous system. Some call it your “second brain.” It doesn’t think like your brain does. But it sends and receives signals constantly.
The main cable connecting these two systems is the vagus nerve. Here’s the surprising part. About 80% of the signals on this nerve travel from your gut UP to your brain, not the other way around.
Your gut bacteria also produce neurotransmitters. Including serotonin, the chemical closely tied to mood and calm. In fact, gut bacteria manufacture roughly 95% of your body’s serotonin supply.
Dr. Emeran Mayer, gastroenterologist at UCLA, put it plainly: “It’s almost unthinkable that the gut is not playing a critical role in mind states.”
Research on this topic has exploded. Publications on gut microbiota and anxiety nearly doubled between 2019 and 2023. This is real science, and it’s growing fast.
How an Unhealthy Gut Creates an Anxious Brain
Think about the last time you felt nervous before something stressful. Your stomach probably felt tight or uneasy. That’s the gut-brain connection working in real time.

But this system can also work against you. When the balance of bacteria in your gut gets disrupted, it’s called gut dysbiosis. And it’s more common than you think.
Dysbiosis triggers low-grade inflammation throughout your body. That inflammation affects the same brain chemicals that regulate your mood, including serotonin and GABA. Less of these chemicals means more anxiety, irritability, and low mood.
What causes dysbiosis? Things most of us do regularly. Eating ultra-processed foods. Chronic stress. Using antibiotics repeatedly. Drinking too much alcohol. Not sleeping enough. Eating too little fibre.

There’s also a painful loop here. Bad diet leads to dysbiosis. Dysbiosis lowers serotonin. Lower serotonin worsens mood. Worse mood leads to stress eating. And stress eating makes the gut worse again.
Mood and anxiety disorders have increased by more than 50% globally in the last three decades. That’s not just stress. That’s biology. And your gut is part of the explanation.
The good news? This loop runs both ways. Fix the gut, and you begin to break the cycle.
The Vagus Nerve — Your Body’s Built-In Calm Switch
Your vagus nerve is the longest cranial nerve in your body. It starts at your brainstem and runs all the way down to your gut, heart, and lungs.
Think of it as your body’s off switch for stress. When it works well, you shift out of “fight or flight” mode and into “rest and digest” mode. When it doesn’t work well, you stay stuck in stress mode, even when there’s no real danger.
Here’s what makes this matter for anxiety. About 80% of the vagus nerve’s fibres are sensory. They carry information from your body up to your brain. So if your gut is inflamed, your brain receives “danger” signals. That can show up as social anxiety, constant worry, or low mood.
The strength of your vagus nerve is called vagal tone. Higher vagal tone means better stress recovery and lower resting anxiety.
You can improve it. Here are four exercises that work, and you can feel results within minutes.
🌿 Nervous System Reset
Extended Exhale
Inhale 4s, Exhale 8s. Do 5 rounds. This immediately pushes your body out of fight-or-flight mode.
Cold Splash
Splash cold water on your face or do 10-20s cool shower. Triggers a reflex that slows your heart rate.
Hum or Gargle
Hum 1-2 mins or gargle water. The vibration directly activates the vagal branches in your throat.
Slow Movement
Yoga, tai chi, or a 10-min slow walk. Gentle, mindful movement actively stimulates the vagus nerve.
Daily practice for 2–8 weeks produces lasting improvements in heart rate variability (HRV) — the most practical measure of vagal tone you can track at home with a wearable.
Probiotics, Prebiotics, and Psychobiotics — What the Research Shows
The probiotic market is full of big claims. Most of them are vague. Here’s what the actual science says, as of 2025.
A term called “psychobiotics” refers to live bacteria that produce a real mental health benefit when you consume enough of them. This isn’t marketing — it’s a clinical term backed by research.
Multiple meta-analyses from 2025 (including Asad et al. in Nutrition Reviews, and Zandifar et al. in Brain and Behavior) show that taking probiotics for 4, 8, and 12 weeks reduces anxiety and depression symptoms in clinically diagnosed patients compared to placebo.
Gut bacteria can break down glutamate to produce GABA and support serotonin. Both of these chemicals reduce anxiety and low mood. The most studied strains for anxiety are Lactobacillus rhamnosus, Lactobacillus helveticus, and Bifidobacterium longum.
But here’s the honest part. Supplements aren’t a fix if your diet is poor. Food comes first. These fermented foods add live bacteria to your gut naturally: yoghurt with live cultures, kefir, unpasteurised sauerkraut, kimchi, low-sugar kombucha, and miso.
Prebiotics — the fibre that feeds your good bacteria — matter just as much. Eat garlic, onions, oats, bananas, and asparagus regularly.
The Gut-Calming Diet — What to Eat for a Calmer Mind
You don’t need a perfect diet. You need a better one.
The Mediterranean diet is the most researched eating style for both gut health and mental wellbeing. It’s not complicated. More plants. More fish. Less processed food.

Research shows that higher protein and healthy fat intake is linked to lower anxiety and depression. Higher refined carbohydrate intake is linked to higher stress and worse mood. That means cutting ultra-processed snacks matters more than counting calories.
Your gut also needs tryptophan to produce serotonin. Tryptophan-rich foods include eggs, turkey, salmon, oats, sunflower seeds, and dark chocolate.
Diversity is key for your microbiome. Aim for 30 different plant foods per week. That sounds like a lot. Start with ten. Add a new vegetable or grain each week.
Eat more of: colourful vegetables, legumes, whole grains, fermented foods, oily fish, nuts and seeds.
Eat less of: ultra-processed snacks, refined sugar, artificial sweeteners, alcohol, deep-fried food.

Artificial sweeteners are worth a specific mention. They disrupt gut bacteria balance even though they contain no calories. Reduce them where you can.
Sleep, Stress, and Exercise — The Habits That Tie It All Together
Diet and probiotics won’t work as well if the rest of your lifestyle is working against your gut.
The Gut-Body Connection
How your daily lifestyle habits physically alter your digestive system and microbiome.
Sleep Quality
- Poor sleep disrupts your gut microbiome in just a few days.
- A damaged microbiome creates a cycle that further degrades sleep quality.
- Action: Aim for 7–9 hours and keep schedules consistent.
Chronic Stress
- Directly damages the gut lining and severely reduces bacterial diversity.
- Spikes cortisol levels, driving physical digestive damage over time.
- Gut damage plays a direct, physical role in anxiety and depression.
Regular Movement
- Target 150 minutes per week of aerobic movement (even walking).
- Actively lowers cortisol and increases microbiome diversity.
- Physical activity directly stimulates the vagus nerve for better digestion.
Here is a simple 4-week plan to start:
Week 1 — Add one fermented food daily. Do 4-8 breathing before bed. Walk 20 minutes, 3 times a week.
Week 2 — Aim for 20 different plant foods this week. Reduce ultra-processed snacks by half.
Week 3 — Add the cold water face splash each morning. Hum for 2 minutes after waking.
Week 4 — Track your HRV if you have a wearable (Garmin, Fitbit, or Polar H10). Add one 10-minute mindfulness session daily.
You don’t need to do all of this at once. Pick one thing from Week 1 and do it today.
Lastly
Your gut and brain are always talking. Feed the right bacteria. Stimulate the vagus nerve. Sleep well, move regularly, and cut the food that works against you.
Small, consistent steps shift the conversation from anxious to calm. The gut-brain axis is not future science. It is your body’s operating system. And you can work with it starting today.