You climb into bed after a long day. Instead of sleep, your legs start aching. A deep, dull throb that won’t quit. You think, “I must be tired.” But here’s the problem: tired legs feel better when you rest. Circulation-based leg pain often gets worse when you lie down.
That difference matters a lot.
Millions of people ignore this sign every night. They blame a long shift, old age, or too much walking. But the real cause is often something going on inside your blood vessels, not your muscles.
In this article, you’ll learn why nighttime makes circulation problems worse. You’ll learn the real conditions behind the pain. And you’ll get specific steps you can take tonight to feel better.
Why Your Legs Hurt More at Night (Not Less)

Think of your calves as a second heart. They squeeze blood back up toward your heart every time you take a step. When you lie still at night, that pump shuts off.
If your vein valves are already weak, blood starts to pool in your lower legs. That pooling builds pressure. That pressure feels like aching, throbbing, or heaviness.
During the day, movement kept things flowing. Your brain was also busy, so you didn’t notice the pain as much. But at night, there’s no movement and no distraction. The ache shows up loud and clear.
Gravity also stops helping at night. When you lie flat, blood has a harder time reaching the legs through the arteries. Some people instinctively dangle their feet off the bed and feel better.

That’s gravity briefly restoring blood flow. It’s a big clue that circulation is the real issue.
Between 25 and 40 percent of women have chronic venous insufficiency. For men, it’s 10 to 20 percent. Many of them don’t know it yet.
The Real Conditions Causing This Pain
Dr. Alan M. Dietzek, Chair of Vascular Surgery at Hackensack Meridian Health, says it plainly: “When people use the phrase ‘poor circulation,’ it can mean different things.” He’s right. There are three main causes of nighttime leg pain from circulation.
Leg Circulation & Night Pain
PAD
Peripheral Artery Disease occurs when plaque narrows arteries. Blood can’t get through. Pain starts during walks, moves to rest, then hits at night.
CVI
Chronic Venous Insufficiency happens when vein valves weaken. Blood pools, causing aching, swelling, and throbbing, especially at night.
Varicose Veins
Not just a cosmetic issue! They cause real cramping & restlessness at night, heavily triggered if you’ve been on your feet all day.
RLS
Restless Legs Syndrome is linked to poor circulation. You feel a constant urge to move your legs, particularly when trying to sleep.
Here’s the key test: tired legs get better with rest. Circulation-based pain either stays the same or gets worse at rest. That’s how you know the difference.
Warning Signs You Should Not Ignore
Some signs tell you this is beyond a home remedy. Pay attention to these.
The gravity test. You dangle your feet over the bed. The pain gets better. That’s not a cramp. That’s an arterial sign.
Skin changes. Look at your ankles, toes, and lower legs. If the skin looks pale, bluish, or reddish, or feels shiny and thin, your circulation is struggling.
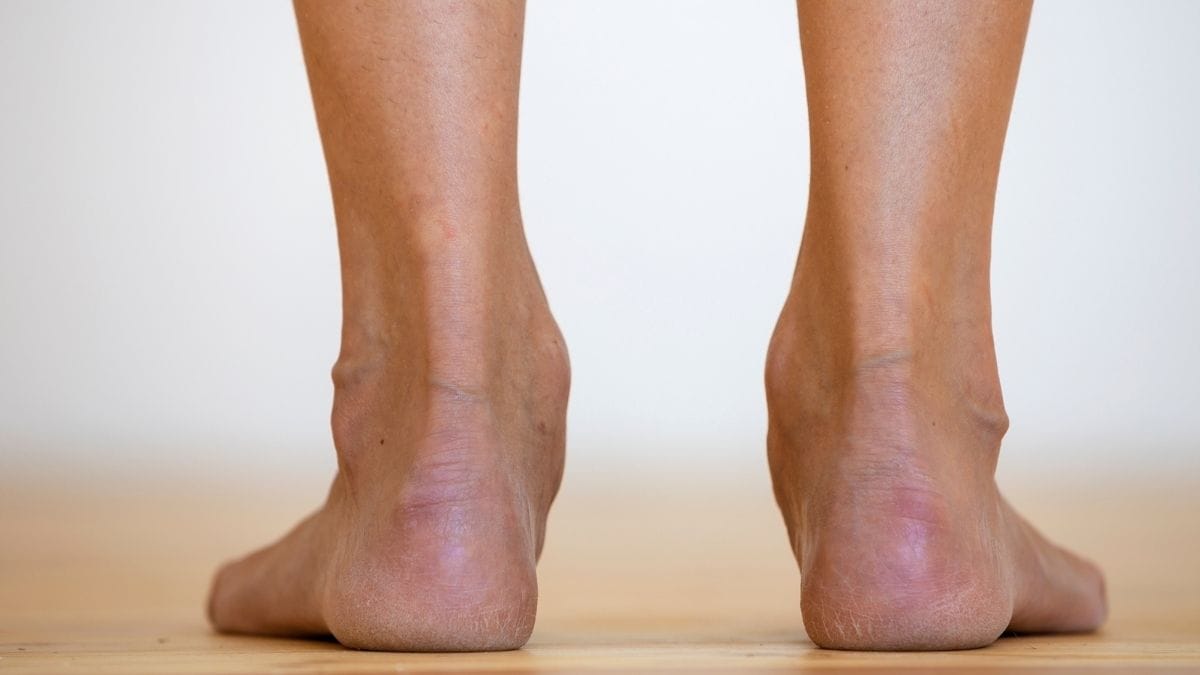
Slow-healing cuts. A small blister or cut that takes weeks to close is a red flag. Healthy blood flow is what heals wounds.
Pain that keeps getting worse week after week. Not just on bad days, but consistently worse over time.
See a doctor this week if you notice:
- Leg pain that worsens at rest or at night
- Cold toes or feet that don’t warm up
- Skin discoloration around the ankles or toes
- A sore or wound on your foot that won’t heal
- Sudden swelling, redness, and warmth in one leg. Go today, as that could be a blood clot
What You Can Do Tonight
Good news: several of these steps cost nothing and work fast.
6 Steps to Soothe Nighttime Leg Pain
1. Elevate Right
A pillow under knees isn’t enough! Keep your calves 12 inches above heart level using a firm wedge.
2. Ankle Pumps
Lie on your back and flex feet up & down 10x. This manually activates your calf pump before sleep.
3. Warm Bath
Soak for 15 minutes and massage your calves to loosen tight vessels and fall asleep faster.
4. Uncross Legs
Crossing compresses veins! Keep feet flat on the floor and shift position every 30 mins in the evening.
5. Hydrate
Dehydration makes blood thicker and flow slower. Drink more water to prevent nighttime symptoms.
6. No Heat Pads
If your feet are numb, you won’t feel a burn. Use warm socks instead of heating pads!
Research shows that regular stretching cuts nighttime leg cramps by up to 45 percent.
Long-Term Habits That Actually Help Your Circulation
Dr. Deborah Hornacek, Vascular Medicine Specialist at Cleveland Clinic, explains it simply: “When your arteries sense exercise, they increase the release of nitric oxide, which relaxes blood vessels and improves blood flow.”
Walking is the best tool you have. You don’t need a gym. Twenty minutes a day at any pace makes a real difference. Your calf muscles squeeze the veins with every step and push blood back to your heart.

Eat for your blood vessels. Beets and leafy greens make nitric oxide, which is good for vessels. Berries, dark chocolate, and pomegranate juice carry polyphenols that protect vessel walls. Fatty fish reduce inflammation. Garlic and turmeric support blood flow.
Try compression stockings, but get the right size. These socks gently squeeze your legs to push blood upward. Talk to your doctor first. Wrong sizing causes more problems than it solves.
Quit smoking. Tobacco is one of the top risk factors for PAD. It damages blood vessels from the inside out.
Move at your desk every 30 to 60 minutes. Sitting still for hours slows leg circulation fast.
When Home Habits Are Not Enough
Lifestyle changes help. They manage symptoms. But they do not fix damaged vein valves, narrowed arteries, or blood clots. Those need a professional eye.
A vascular evaluation is not scary. It often starts with a venous ultrasound, which is painless and non-invasive, done in a clinic. The doctor checks blood flow, valve function, and vein shape in real time.
Modern vein treatments are minimally invasive. Many are covered by insurance. They address the root cause in ways that stretching and elevation simply cannot.
If your symptoms have lasted more than two to three weeks, or if they match the warning signs above, book a vascular assessment. You are not overreacting. You are paying attention to something that matters.